In this article:
- The Nutrition Arsenal – Foods That Actually Move the Needle & the Vitamin C fallacy
- Exercise – Your Immune System’s Personal Trainer
- The Foundation Pillars – Sleep, Hydration & Lifestyle Factors
- Seasonal Immune Strategy – Your Fall/Winter Game Plan
- Integration – Weaving Physical and Mental Practices
Building Your Body’s Fortress of Health

Picture your immune system as a medieval fortress. Last week, in the Mental Immunity article, we trained the sentries on the walls—your mind—to spot threats early and maintain calm during siege conditions. This week we’ll upgrade the fortress walls, reinforcing the armory, and ensuring your body’s defense infrastructure can withstand anything winter throws at it.
Last week we discussed how to turn your anxious mind into a serenity safe haven. Now let’s give your body the same upgrade—without requiring a nutrition PhD or Olympic training regimen. Because here’s the thing: most “immune boosting” advice floating around social media is about as scientifically sound as medieval leech therapy.
I have my own therapies I use to help sustain me through the season of sickness. I stay with a holistic approach to anything I add to my body. There are some things I take as prevention and other items I employ once sickness starts to take hold. Here I want to provide some science-backed physical strategies that work within real-world constraints. No expensive superfoods that cost that cut into your budget. No workout routines that require personal trainer supervision. Just evidence-based practices that fit into actual human schedules and funds.

Here’s what might surprise you: that morning smoothie packed with “immune-boosting” ingredients could actually be sabotaging your fortress if you’re drinking it at the wrong time. Timing, it turns out, matters more than most ingredients. And that high-intensity workout you’ve been pushing through while stressed? It might be opening the castle gates to invaders rather than strengthening the guards.
This week, we’re building on your newfound mental resilience with physical practices that have actual peer-reviewed pedigree. We’ll explore the nutrition arsenal that moves the needle (it’s not what Instagram influencers claim), exercise prescriptions that enhance rather than suppress immunity, and lifestyle factors with measurable benefits.
By the end of this week, you’ll have a stronger fortress—mind and body working in harmony to create a defense system that will keep you out of doctors’ offices and strengthen not only your immune system but also, your mind and body.
Section 1: The Nutrition Arsenal – Foods That Actually Move the Needle
- The Immune-Nutrition Connection: Beyond Vitamin C
Most people treat immune nutrition like tossing supplements at a wall and hoping something sticks. The reality? About 95% of Americans are deficient in vitamin D, 84% in vitamin E, and 45% in vitamin A—nutrients with actual clinical evidence for immune function. Reference study – Inadequacy of Immune Health Nutrients.
The immune-nutrition connection operates through several key mechanisms. Certain nutrients serve as cofactors for immune cell development, while others directly modulate inflammatory pathways. But here’s where it gets interesting: the same nutrient can be pro-inflammatory or anti-inflammatory depending on timing, dose, and what else you’re eating.
The Reality Check: Most “immune-boosting” foods are marketing fiction. Much like most marketing campaigns. Your immune system doesn’t need boosting—it needs balancing. I can’t encourage enough, read the labels. Along with that, there are many simple things we can do to assure we are balanced. Think of it like tuning a guitar rather than cranking the amplifier to eleven.
The Big Three nutrients with actual clinical evidence are Vitamin D (regulates both innate and adaptive immunity), Zinc (essential for immune cell development), and Vitamin A (critical for mucosal immunity—your first line of defense). Everything else is supporting cast.

Although, pop science leads us to believe that Vitamin C is standard for boosting the immune system and front-line defender in cold / flu prevention.
Actual studies reveal king C to be something other than the king. In Vitamin C for preventing and treating the common cold. Cochrane Database of Systematic Reviews and Vitamin C for preventing and treating the common cold. The authors conclude “The failure of vitamin C supplementation to reduce the incidence of colds in the general population indicates that routine vitamin C supplementation is not justified, yet vitamin C may be useful for people exposed to brief periods of severe physical exercise. Regular supplementation trials have shown that vitamin C reduces the duration of colds, but this was not replicated in the few therapeutic trials that have been carried out. Nevertheless, given the consistent effect of vitamin C on the duration and severity of colds in the regular supplementation studies, and the low cost and safety, it may be worthwhile for common cold patients to test on an individual basis whether therapeutic vitamin C is beneficial for them. Further therapeutic RCTs are warranted”. The definitive Cochrane Review (Hemilä & Chalker, 2013) analyzing 29 trials with 11,306 participants found vitamin C supplementation had essentially no effect on cold prevention in the general population (RR 0.97), while showing significant benefits only for people under extreme physical stress like marathon runners and soldiers (RR 0.48, representing a 52% reduction in cold incidence).”
Ultimately, Vitamin C is not bad for you and large intake is not harmful, but it is not the most effective cold suppressant or preventative. Large doses can upset your stomach. I’ve experienced this because I lived by the myth that vitamin C could stop a cold.
Vitamin C is good for collagen production, healing wounds, providing healthy skin, antioxidant, supports blood vessel function and heart function. But, in conclusion not so great for cold prevention

Another common immune booster is Echinacea. A plant found in the United States. It does have a modest preventative force of cold impact. In Echinacea Reduces Antibiotics by Preventing Respiratory Infections: A Meta-Analysis (ERA-PRIMA), reduced respiratory infections by up 25% to 32% and cut antibiotic use by 40%. I get on the echinacea routine occasionally. I use it much like the science disposes, sort of a turbocharger for my immunity system. Studies are indicative that this plant is best as a preventative moreover than a treatment. Once your in grip of your illness, echinacea won’t necessarily be the one to release you from it. Along with cold prevention, the study Echinacea Reduces Antibiotics by Preventing Respiratory Infections shows its ability to reduce the need for antibiotics. It reduced the monthly RTI occurrence. Overall it reduced RTI’s by 32%, provided fewer complications (56% reduction in pneumonia, ear infections and the like) and yielded a 40% reduction in the need for antibiotic use. So, echinacea may not be a cure but there are good indications that it can be a preventative if dosed as recommended. It’s recommended to take it for a few weeks, then stop for a couple weeks before dosing again. This is most likely because extensive uptake reduces the effectiveness, and your body can’t take on any more to be effective.
I want to add one personal protocol I subscribe to when I sense a cold coming on. Which is, coating my sinuses with zinc. Just before bedtime, I take either candied zinc or some of the more soluble forms in a compressed powder form. I take it and do not swallow it but suck on it. I allow it to saturate my sinuses and then sleep on it. When I do this at the very forefront of a virus trying to seat itself in me, I have been able to either completely eliminate any cold virus or at least kept the symptoms very minimal AND those symptoms last one or two days, then it’s gone. If I do this once the cold takes hold it’s of no use. I need to catch it at the very beginning. When I get that timing, I have 100% success of minimal or no cold symptoms.
1.2 Power Foods with Peer-Reviewed Pedigree
Fermented Foods & Microbiome Warriors
Your gut houses 70% of your immune system, which includes T cells, B cells, plasma cells, macrophages, and dendritic cells. These cells are constantly sampling what comes through your digestive tract. It consists of 400 square meters (size of a tennis court) exposed to the outside world. Which comes in as food, bacteria, toxin and pathogens all passing through. It must distinguish helpful microbes from harmful ones. Essentially, making your microbiome the most important army you’ve never thought about. Your gut immune system communicates with and influences immune function throughout your entire body. Gut immune cells travel to other parts of the body. Inflammatory signals from the gut affect systemic immunity.
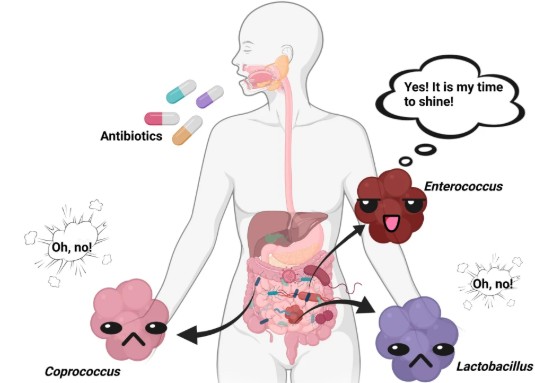
More on antibiotics, here as well, they disrupt the generation of the gut microbiome and shuts it down. The antibiotic takes over to attack the infection, while, also, depleting the gut of its useful service. That’s why your stomach experiences pain, cramps, diarrhea and other discomforts during the antibiotic enforcement. It also leaves in its tract a need for gut healing once the dosing is complete. More bad news on antibiotics. Avoid them whenever you can. I have worked diligently to get myself off antibiotics and I feel soooohhh much better that I have. I was once a two times per year sinus infection carrier. Always taking in the antibiotics. Then I got into a more stringent sinus cleansing process and I now pass right through any use of antibiotics. And, I am feeling sooooohhhh much better in mind, body and spirit. It is vital to keep your gut healthy.
Getting back to good gut foods. A 2019 systematic review analyzing 24 randomized controlled trials with 1,886 participants found that fermented foods produced significant improvements in inflammatory markers and pathogen resistance.
The methodology was rigorous: 4-12 week interventions comparing fermented food consumption to controls, measuring inflammatory cytokines, pathogen resistance, and immune cell activity. Results showed consistent improvements across multiple immune parameters.
The “Rule of 3” Protocol: Three different fermented foods, three times per week. This isn’t about chugging kombucha until you’re buzzed from the alcohol content. It’s about diversity and consistency.
Your Shopping List (with quality markers):
- Kefir: Look for live cultures and minimal sugar
- Sauerkraut: Refrigerated section, no vinegar in ingredients
- Miso: Unpasteurized, aged at least 6 months
The key is variety. Different fermented foods introduce different bacterial strains, creating a more resilient microbiome ecosystem. Good clean, Greek yogurt has many good gut benefits, as well. But be sure it’s Greek with no other additives. I also take a probiotic once per day to help along, in parallel.
Polyphenol Powerhouses
Polyphenols modulate immune function through multiple pathways, including antioxidant activity and direct effects on immune cell signaling. But here’s the twist: it’s not about individual “superfoods.” It’s about eating across the color spectrum.
The Color Strategy: Each color represents different polyphenol families. Purple foods contain anthocyanins, orange foods have carotenoids, green foods provide catechins. Your immune system benefits from the full spectrum, not just one class.
Daily Polyphenol Targets:

- Purple: blueberries, red cabbage, purple onions
- Orange: sweet potatoes, carrots, turmeric
- Green: green tea, broccoli, spinach
- Red: tomatoes, red peppers, pomegranate
- Brown: cocoa, this is my personal favorite; it is rich in Flavanols and Phenolics. Darker is better. I put a small amount of pure cocoa into my coffee. Careful, though too much can upset some people’s stomach
The “Purple Power Hour”: Consuming polyphenol-rich foods 30-60 minutes before meals maximizes absorption and minimizes blood sugar spikes that can temporarily suppress immune function.
Mushroom Medicine
Beta-glucans found in mushrooms have been shown to enhance immune cell activity, but not all mushrooms are created equal. There are specific varieties with measurable beta-glucan content.

The Magnificent Seven (evidence-backed varieties):
- Shiitake: Contains lentinan, shown to enhance T-cell function. T-lymphocytes (T-cells) are white blood cells that mature in the thymus (hence the “T”). They’re part of your adaptive immune system – the sophisticated, targeted immune response. They have memory – can remember and respond faster to previously encountered threats Maitake: Rich in D-fraction beta-glucans, enhance immune strength
- Reishi: Adaptogenic properties for stress-immune connection
- Turkey tail: High in PSK polysaccharides, provides T-cell stimulation
- Cordyceps: Supports cellular energy and immune function
- Lion’s mane: Nervous system support (immune-brain connection)
- Chaga: High ORAC (Oxygen Radical Absorbance Capacity) antioxidant values. It’s a laboratory method that was used to measure the antioxidant capacity of foods and supplements
Fresh vs. Supplement Strategy: Fresh mushrooms provide broader nutritional profiles, while standardized extracts deliver concentrated active compounds. Use fresh varieties 3-4x per week, consider extracts during high-stress periods.
Reality Check: Mushroom coffee probably won’t save you. The concentration of active compounds in most commercial mushroom blends is too low to provide therapeutic benefits. I am a proponent of getting it direct from the source. No additional processing and/or drying out procedures, additives or shelf degradation.
1.3 Nutrient Timing: When You Eat Matters More Than You Think
Immune parameters like pro-inflammatory cytokine production exhibit peaks during early nocturnal sleep, while anti-inflammatory activity peaks during daytime wakefulness. This circadian immune rhythm means timing your nutrition strategically.
The Circadian Immune Connection: Your immune system operates on a 24-hour cycle. Eating inflammatory foods late in the day disrupts this rhythm, while consuming anti-inflammatory nutrients at specific times enhances immune function.
The 3-2-1 Eating Strategy:
- 3 hours before sleep: Stop eating to allow immune-supporting growth hormone release
- 2 servings of polyphenol-rich foods with morning and afternoon meals
- 1 serving of fermented food daily, preferably with lunch for optimal microbiome benefits
Integration Point: This connects perfectly with the mindful eating practices from Week 1. Use your established awareness to notice how different foods affect your energy and sleep quality.
1.4 Foods That Sabotage Your Fortress
The Usual Suspects with specific thresholds:

- Processed foods: More than 20% of daily calories from ultra-processed foods correlates with increased inflammatory markers. Read the labels. You can tell it’s bad 98% of the time if the ingredients doesn’t make sense and/or if it contains multiple syllables
- Excess sugar: >25g added sugar daily suppresses white blood cell function for up to 5 hours. Reality shows us that sugar, especially refined, process sugar has no nutritional value and in fact is a detriment to good health. It ain’t easy to do but drop it from your diet if you can. I did, just by finding out that cancer actually feeds off sugar. That was an inspiration to me to get it outta my system
- Refined oils: High omega-6 to omega-3 ratios (>10:1) promote inflammatory pathways. Omega 6 = BAD, which are corn oil, safflower oil, sesame oil, soybean and sunflower oils. Omega 3 = GOOD, which are flaxseed, chia, hemp, walnut, fish, algae and krill oils. Also best for cooking are, extra virgin olive oil, avocado oil, macadamia oil, coconut oil, butter/ghee, tallow
Some Other Considerations – Hidden Immune Disruptors:
- Seed oils in restaurant food: Often oxidized from high-heat cooking
- Artificial additives: Emulsifiers can disrupt gut barrier function
- Alcohol timing: Consuming within 3 hours of sleep disrupts immune-supporting sleep stages
The 80/20 Reality: Perfect nutrition is the enemy of good nutrition. Focus on getting the fundamentals right 80% of the time rather than obsessing over perfection.
Section 1 Quick-Win Takeaways:
- Daily Dozen Checklist: 3 colors of vegetables, 1 fermented food, 1 serving omega-3 rich food
- Timing Template: Polyphenols with meals, stop eating 3 hours before sleep
- Emergency Protocol: When stress is high, prioritize fermented foods and reduce inflammatory foods
Section 2: Exercise – Your Immune System’s Personal Trainer
2.1 The Exercise-Immunity Paradox
Here’s the paradox that confuses most people: exercise simultaneously strengthens and temporarily weakens your immune system. The key is understanding the J-curve relationship between exercise intensity and immune function.
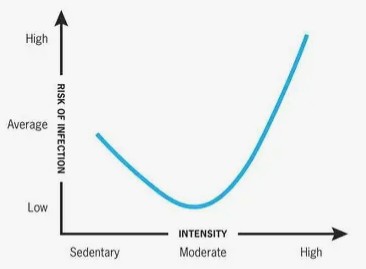
The J-Curve Explained: Sedentary people have baseline immune function. Moderate exercisers see enhanced immunity. But push into exhaustive exercise territory, and immune function temporarily dips below baseline—the “open window” where you’re more susceptible to infection.
Research comparing moderate continuous training to high-intensity interval training found that moderate intensity improved immune cell counts, while HIIT (High Intensity Interval Training) temporarily suppressed them. This isn’t anti-HIIT propaganda—it’s about strategic timing. Moderation shows to be the best approach to exercise for establishing a strong anti-viral, anti-infectious immune system.
Research consistently shows moderate exercise enhances immune function. One epidemiological study meta-analysis of 23 studies with over 3000 participants, found that people engaging in aerobic exercise 5+ days per week had 43% fewer days with upper respiratory infections compared to minimally active individuals (Nieman et al., 2011). A systemic review (Chastin et al., 2021) found no detrimental immune effects from regular physical activity up to moderate-to-vigorous intensity (60-600 minutes per week). While the J-curve relationship shows that prolonged, intense exercise causes immunosuppression and moderate intensity exercise improves immune function. So, a good immune enhancement target is 60 to 600 minutes per week. Keep in mind that overexertion during any single exercise can potentially be detrimental to your body. Prolonged, intense exercise causes immunosuppression (Exercise and Respiratory Tract Viral Infections – PMC) and creates what researchers call an “open window” where your immune system is temporarily weakened for 3-72 hours after intense exercise.
Intense exercise can be summarized as; sustained effort of >85% max heart rate for >60 minutes OR moderate-high intensity for >90 minutes OR exercising to the point of voluntary exhaustion regardless of duration.
2.2 The Goldilocks Zone: Exercise Prescriptions That Work
Moderate Cardio Magic – Running, Biking, Skating, Skiing, Swimming, Walking, etc.
The research consistently shows benefits from 150 minutes of moderate-intensity activity per week—basically the standard public health recommendation, but now with immune-specific backing.
What “Moderate” Actually Means:
- Can maintain conversation but breathing is slightly elevated
- 60-70% of age-predicted max heart rate
- Rate of Perceived Exertion: 5-6 out of 10
The 150-Minute Weekly Template:
- Option 1: 30 minutes, 5 days per week
- Option 2: 25 minutes, 6 days per week (allows one full rest day)
- Option 3: 3 longer sessions (45-50 minutes) with rest days between
Exercise Banking: Life happens. Research shows you can bank moderate exercise benefits. If you miss weekday sessions, longer weekend sessions can partially compensate—just avoid the “weekend warrior” extreme that tips into immune suppression.
Integration Point: Combine this with Week 1’s mindfulness practices. Walking meditation, mindful swimming, or awareness-based cycling turn exercise into dual-purpose mind-body medicine.

I used to run or jog 3 to 5 miles daily. Over time I came to realize the impact on my joints was eventually going to be detrimental. I thoroughly enjoyed kickin’ up the step and running with my dog. We both had some good exercise. However, I was continually contemplating, while pounding on the pavement or ground, how that would wear on my connecting joints. Eventually, I stopped the jog and picked up walking. My personal favorite is walking in a forest, listening to the surrounding critters, taking in the scent of pine and flowers or getting hit by a descending acorn from the oak tree canopy. I had one direct hit on my thumb knuckle. What a good shot. Nonetheless, not only do I help my body, during my hikes; included also is my mindfulness staying focused on the environment around me. Mind and body in synch.
Strength Training for Immune Strength
Resistance training appears in multiple studies as beneficial for immune function, particularly for aging adults where immune function naturally declines.
The Minimum Effective Dose: Two sessions per week targeting major muscle groups. This isn’t about bodybuilder splits—it’s about stimulating enough muscle tissue to trigger beneficial immune adaptations without excessive stress.
Bodyweight Immunity Routine (for busy schedules):

- Upper Body: Push-ups, pike push-ups, tricep dips
- Lower Body: Squats, lunges, single-leg deadlifts
- Core/Stability: Planks, side planks, dead bugs
- Protocol: 2-3 sets, 8-15 reps, 2x per week
Reality Check: More isn’t always better. Prolonged intensive training can depress immunity through elevated stress hormones. Listen to your body’s recovery signals.
Weight training and cardio benefit the immune system through complementary mechanisms. Weight training is particularly valuable for preserving immune function with aging and providing efficient immune benefits, while cardio excels at systemic circulation and stress resilience.
How Exercise Benefits the Immune System
Immune Cell Circulation
- Increased blood flow rapidly mobilizes immune cells from lymphoid organs
- Natural killer (NK) cells increase by 50-300% during moderate exercise
- Neutrophils and lymphocytes are redistributed from storage sites to circulation
- Enhanced immune surveillance – more immune cells patrolling for threat
Anti-Inflammatory Effects
- Better blood flow to immune organs (spleen, lymph nodes, bone marrow)
- Improved waste removal from tissues
- Increased tissue oxygenation supporting immune cell metabolism
Enhance Immune Training and Memory
Improved lymph flow helps transport antigens to lymph nodes
- T-cell priming – more effective immune memory formati
- Blood flow increase provides immune cells to patrol effectively
Neuro Level Optimization
- Improved stress hormone balance – better cortisol patterns
- Enhanced parasympathetic tone – supports immune recovery
- Reduced chronic stress responses that suppress immunity
- Better sleep quality – crucial for immune function
Glucose and Lipid Metabolism
- Improved insulin sensitivity – better fuel delivery to immune cells
- Healthier lipid profiles support cell membrane function
- Reduced metabolic inflammation that can impair immunity
- Better nutrient utilization for immune system needs
Gut Health Enhancement
- Increased gut microbiome diversity – supports immune training
- Enhanced short-chain fatty acid production – fuel for immune cells
- Improved gut barrier integrity – prevents inflammatory responses
- Better gut-brain-immune communication
Cardiovascular and Circulatory Benefits
- Enhanced capillary density – better nutrient/oxygen delivery
- Improved cardiac output – more efficient circulation
- Lower resting blood pressure – reduced cardiovascular stress
- Better gut-brain-immune communication
- Improved lymphatic drainage – better toxin removal
- Enhanced lymph node function – more effective immune processing
Better fluid balance – supports immune cell mobility
In summary, get the blood flowing. A stagnate life = limited blood circulation = cellular morbidity = immune system depression = a multitude of ailments. Stay as active as you possibly can. As we’ve discussed you don’t need to overexert but you should get some level of moderate exercise or activity. Extended days spent couching, lounging or TVing are not conducive to building good seasonal immunity or just any immunity. I am all about days for rest because they help to re-generate the body and mind. And, they should be used for re-generation, not necessarily as a lifestyle.
2.3 Exercise Timing and Seasonal Strategies
Circadian Exercise: Exercise timing affects immune function through circadian rhythm modulation. Morning exercise supports natural cortisol rhythms and promotes better sleep, while late evening exercise can disrupt sleep-immune cycles.
Optimal Timing Windows:
- Morning (7-10 AM): Best for moderate cardio, supports natural energy rhythms
- Afternoon (3-6 PM): Peak strength performance window. This is my time. I start to lose focus after working, so an exercise break brings my head back to clarity and re-energizes me
- Early Evening (6-8 PM): Last window before sleep interference. For me an occasional walk, especially in the woods, is a perfect end of day routine
Seasonal Adjustments:
- Fall: Gradually increase indoor options as daylight decreases
- Winter: Prioritize vitamin D exposure through outdoor morning walks
- Light exposure: Exercise outdoors when possible for circadian and mood benefits
2.4 When NOT to Exercise (Critical for Immune Health)
This might be the most important subsection. Exercise during illness or high stress can amplify immune suppression.
The Illness Exercise Decision Tree:
- Above the neck (sniffles, mild sore throat): Light exercise OK
- Below the neck (chest congestion, body aches): Rest completely
- Fever: Absolute rest until 24 hours fever-free
- Fatigue without other symptoms: Consider stress levels and sleep quality
Overtraining Red Flags:
- Persistent elevated resting heart rate
- Declining performance despite consistent training
- Increased susceptibility to minor illnesses
- Sleep disturbances or mood changes
- Loss of exercise motivation
Recovery Protocols: When returning after illness, start at 50% of previous intensity for the first week, gradually progressing back to full training loads. Engage your mind to listen to your body. Whenever I come off an illness or injury, I’m not getting into my full exercise engagement until I feel my breathing not so labored or my muscles not so weak. It takes a bit of time to get back to normal routines after being out for a bit. I’ve learned to just go with it and not push it. Some recoveries happen quickly, like in a day or two, while others may take 1 to 2 weeks. I’m good with that because my body needs to take some time to catch up with my mind. It all works in synchrony.
Section 2 Quick-Win Takeaways:
- Weekly Template: 150 minutes moderate cardio + 2 strength sessions
- Daily Check-in: Rate energy/stress levels before exercising
- Recovery Signals: Honor fatigue, prioritize sleep over training. However, there are times I just feel exhausted after desking all day and just being immobile. That stagnation can lead me to more stagnation. Those are the times I will push myself to the gym or get in some walk time. And, at the end of those sessions I don’t feel exhausted, I actually feel refreshed and the brain fog has been removed. And if I take my dogs with me, they sleep better, too.
Section 3: The Foundation Pillars – Sleep, Hydration & Lifestyle Factors
3.1 Sleep: Your Immune System’s Overnight Repair Shop
A landmark study of identical twins found that the twin with shorter sleep duration had a depressed immune system compared to their sibling. The genetic control makes this finding particularly compelling—same DNA, different sleep, different immune function.
Sleep affects immune parameters through multiple mechanisms: enhancing T cell function, promoting anti-inflammatory cytokine production, and supporting immunological memory formation. But here’s the critical detail: Research shows that people who sleep less than 6 hours per night are 4.2 times more likely to catch a cold when exposed to rhinovirus compared to those getting 7+ hours.
The Sleep-Immune Connection Breakdown:
- Stages 1-2: Immune cell circulation increases
- Deep Sleep (Stage 3): Growth hormone release, tissue repair, memory consolidation
- REM Sleep: Adaptive immune function, emotional regulation
- Full Cycle: 7-9 hours needed for complete immune restoration
Practical Sleep Optimization
The Sleep Fortress Protocol:

Temperature: Cool environment (65-68°F) supports natural temperature drop that signals sleep onset. Body temperature regulation is crucial for sleep-immune interactions.
Light Management:
- Bright light exposure within 1 hour of waking
- Dim lights 2 hours before intended sleep
- Blue light blocking if screen use is necessary
Timing Consistency: Sleep regularity is as important as duration for immune function. Aim for consistent sleep and wake times within 30 minutes, even on weekends.
Integration with Week 1: Use the evening mindfulness practices to create a buffer between daily stress and sleep. The body scan technique naturally supports the transition into sleep stages.
Troubleshooting Common Disruptors:
- Racing mind: Practice the 4-7-8 breathing technique from Week 1
- Physical tension: Progressive muscle relaxation starting from toes
- Environmental noise: White noise or earplugs, not sleep music that can cause micro-awakenings
3.2 Hydration: The Overlooked Immune Multiplier

Most hydration advice focuses on sports performance, but even mild dehydration can impair immune cell circulation and concentration. Your lymphatic system—a key component of immune function—relies on adequate fluid for proper circulation.
Beyond Water:
- Electrolyte balance: Sodium, potassium, and magnesium support cellular hydration
- Timing matters: Large fluid intake right before sleep disrupts immune-supporting sleep stages
- Quality considerations: Filtered water removes chlorine that can disrupt gut microbiome
The Hydration-Immune Formula: Basic needs: 0.5-1 oz per pound of body weight Add 12-16 oz for every hour of exercise Add 8 oz for every caffeinated drink Adjust for climate and individual variation
Practical Application:
- Morning: 16-20 oz upon waking (rehydration after overnight fast)
- Throughout day: Small, frequent sips rather than large quantities
- Evening: Taper intake 2 hours before sleep
3.3 Lifestyle Factors That Make or Break Your Fortress
Temperature Exposure
Cold and heat exposure create hormetic stress—controlled stress that strengthens adaptive capacity. But the key word is “controlled.”

A large randomized controlled trial with over 3,000 participants found that people who took regular cold showers had a 29% reduction in sickness absence from work PLOS. That’s pretty significant.

Recent 2024 Study: A September 2024 study found that regular cold shower exposure enhances both humoral and cell-mediated immunity through upregulation of antibodies, interleukin-2, and interleukin-4 PubMedScienceDirect. The researchers concluded that brief cold stressors may induce physiological adaptations that prime the immune response ScienceDirect.
Important Context: While meta-analysis showed no significant effects on immune function immediately or 1 hour post-cold water immersion, narrative synthesis suggested longer-term benefits PLOS. This means the immune benefits come from regular practice over time, not immediate effects.
Cold Therapy Protocols:
- Beginner: 30-second cold shower finish, gradually increase duration
- Intermediate: 2-3 minutes cold exposure, 3-4x per week
- Advanced: Ice baths or cold plunging with proper supervision
- Temperature: 45o-59o F (45o-59o C)
- Frequency: studies indicate 30 consecutive days for benefit
- Recommended: the beginner time is shown to be adequate for immune strength
Cold Therapy Who Should Be Cautious:
Recent research has started to suggest decreasing the inflammatory response to temporary illness might prolong or prevent recovery, so this is more about prevention prior to illness moreover, than treatment when already sick.
Special Considerations / Cautionary Notes:
- People with heart conditions (cold causes vasoconstriction)
- During active illness
- Pregnant women (consult doctor)
- People with Raynaud’s syndrome
- Elderly (higher hypothermia risk)
My Personal Approach:
I can’t say I’m advanced, but I do take 5-minute cold showers daily. I don’t just jump in, I go with hot first then, drop it. Not only does it cool me down, it relaxes me as well. I have a specific routine that I can share on another post. It’s been life changing for me.
Sauna Benefits: Regular sauna use shows immune benefits through heat shock protein activation and improved circulation. Add a cold plunge with it and you got a formula for being an immunity superhero.
Temperature Therapy Protocol: 15-20 minutes sauna followed by cool-down period, 2-3x per week. Or alternate hot/cold exposure for greater hormetic effect.
Environmental Toxin Reduction
The Immune Load Concept: Your immune system has limited bandwidth. Environmental toxins compete with pathogens for immune attention, potentially reducing your ability to fight infections.
High-Impact Swaps (focusing on biggest wins):
- Air quality: HEPA filter in bedroom, I just added this. Houseplants that filter VOCs
- Water: Quality filtration system to remove chlorine and heavy metals
- Personal care: Choose products with fewer endocrine disruptors
- Cleaning products: Simple ingredients (vinegar, baking soda) over chemical cocktails
- Food storage: Glass over plastic, especially for acidic or heated foods
Reality Check: Perfect environmental wellness is impossible in modern life. Focus on the 20% of changes that provide 80% of the benefit—air quality, water quality, and reducing plastic exposure to heated foods.
Social Connection (Physical Aspects)

Physical touch and social interaction have measurable immune benefits. Research shows that people with strong social connections have 50% lower mortality risk, partly through immune-mediated pathways.
Touch and Immunity: Physical affection increases oxytocin and decreases cortisol, creating a hormonal environment that supports immune function. This isn’t just romantic touch—platonic hugs, pet interactions, and even massage show benefits.
Community Activities: Group exercise, community gardening, or team sports provide both physical activity and social connection benefits. The combination amplifies immune benefits beyond either factor alone.
Integration Point: Combine social activities with physical practices from this week. Walking groups, cooking classes focused on immune-supporting foods, or outdoor activities that provide exercise, light exposure, and social connection.
Get connected, find a group or function you resonate with. Just step into it, if nothing else for curiosities sake. Don’t assume you have all the answers or that people are all bad. As I go through this walk of life, I come across more I don’t know than what I do know. Also, once being stone engraved in a cycle of cynicism I’ve come to realize not all people have bad intentions and most want to connect, share parts of themselves and find points of common ground.
Section 3 Quick-Win Takeaways:
- Sleep Checklist: 7-9 hours, consistent timing, cool/dark environment
- Hydration Template: Front-load morning hydration, taper evening intake
- Environmental Priorities: Air quality, water quality, reduce plastic exposure
- Connection: get together with people, communicate, listen, share
Section 4: Seasonal Immune Strategy – Your Fall/Winter Game Plan
4.1 The Seasonal Immune Shift
Your immune system doesn’t just respond to pathogens—it anticipates seasonal challenges. Research shows that immune gene expression changes with seasons, with inflammation-related genes more active in winter months. This isn’t just correlation; it’s evolutionary preparation for seasonal viral patterns.
Here’s some real reasons we get sick in winter:
- Reduced sunlight: Vitamin D deficiency peaks in late winter
- Indoor crowding: Closer contact facilitates transmission
- Dry air: Compromises nasal mucosal barriers
- Circadian disruption: Shorter days affect sleep-immune cycles
- Stress accumulation: Holiday stress + reduced outdoor time
Preparation vs. Reaction: Most people wait until they feel something coming on. Smart immune strategy starts in early fall, building resilience before seasonal challenges peak.
4.2 Fall Preparation Protocol
Nutrition Adjustments
Seasonal Superfoods (available and affordable in fall):
- Pumpkin: High in vitamin A for mucosal immunity
- Sweet potatoes: Beta-carotene and fiber for gut health
- Apples: Quercetin, a natural antihistamine
- Cranberries: Proanthocyanidins for urinary tract health
- Winter squash: Multiple carotenoids and immune-supporting minerals
Vitamin D Strategy: This is non-negotiable for fall/winter immune health.
- Testing: Get baseline 25(OH)D levels in early fall
- Supplementation: Most adults need 2000-4000 IU daily in winter
- Food sources: Fatty fish, egg yolks, fortified foods
- Sun exposure: 10-15 minutes midday sun when possible
Warming Foods Philosophy: Traditional medicine systems emphasize “warming” foods in cold seasons. Modern science supports this through thermogenesis and circulation benefits.
- Spices: Ginger, turmeric, cinnamon boost circulation and have anti-inflammatory properties
- Warm preparations: Soups, stews, and warm teas support hydration and nutrient absorption
- Root vegetables: Grounding foods that support steady energy
Exercise Evolution
Indoor Workout Transitions: Don’t wait for the first blizzard to figure out your indoor exercise routine.
- Home equipment basics: Resistance bands, yoga mat, light weights
- Bodyweight circuits: No equipment needed, can be done in small spaces
- Online resources: Establish go-to video channels or apps before you need them
Seasonal Movement Activities:
- Hiking: Fall weather is perfect for immune-boosting outdoor exercise
- Raking leaves: Functional fitness that serves multiple purposes
- Walking meetings: Maintain outdoor time despite shorter days
- Indoor rock climbing: Social, challenging, builds strength
Light Exposure Strategy: Critical for maintaining circadian rhythms and mood.
- Morning walks: Even 10 minutes helps maintain circadian alignment
- Light therapy: Consider a 10,000 lux light box for early morning use
- Bright indoor spaces: Work and exercise near windows when possible
4.3 Winter Maintenance Mode
The Immune Maintenance Matrix:
Daily Practices:
- Morning light exposure (10 minutes minimum)
- Immune-supporting breakfast (protein + polyphenols)
- Movement practice (even 15 minutes counts)
- Evening wind-down routine from Week 1
Weekly Practices:
- 2-3 strength training sessions
- 1-2 longer cardio sessions
- Social connection activities
- Meal prep including fermented foods
Monthly Practices:
- Vitamin D level check (if supplementing)
- Stress assessment and adjustment of practices
- Review and adjust exercise routine for motivation
- Environmental health check (air quality, sleep environment)
Holiday Survival: Maintaining immune practices during social seasons.
- Travel strategy: Portable immune toolkit (hand sanitizer, immune-supporting snacks, travel-size supplements)
- Social eating: Focus on vegetables and protein, moderate alcohol and sugar
- Sleep protection: Maintain sleep schedule despite social pressure
- Stress management: Use Week 1 techniques during family gatherings
Travel and Immunity:
- Hydration: Airplane air is extremely dry; drink extra water
- Movement: Walk during layovers, stretch on long flights
- Hand hygiene: Most important prevention strategy
- Sleep adjustment: Gradually shift sleep schedule before travel
4.4 Spring Reset Preparation
Transition Planning: Seasonal changes are stressful on the immune system. Plan the transition rather than letting it happen to you.
Assessment Tools:
- Energy levels: How did your winter practices affect daily energy?
- Illness frequency: Track any infections and recovery time
- Sleep quality: Note seasonal patterns in sleep needs
- Exercise consistency: What worked and what didn’t during low-motivation periods?
Spring Adjustments:
- Gradual increase: Build outdoor exercise as weather permits
- Vitamin D tapering: Reduce supplementation as sun exposure increases
- Seasonal foods: Transition to spring vegetables and lighter preparations
- Social reintegration: Increase group activities as outdoor options expand
Section 4 Quick-Win Takeaways:
- Fall Checklist: Vitamin D testing, indoor exercise plan, immune-supporting seasonal foods
- Winter Toolkit: Light therapy, social connection, travel immune strategies
- Spring Assessment: Review what worked, plan adjustments for the coming year
Section 5: Integration – Weaving Physical and Mental Practices
5.1 The Mind-Body Immune Connection in Action
Here’s where the magic happens: your Week 1 mental practices and Week 2 physical strategies aren’t separate interventions—they’re components of an integrated system that amplifies immune function beyond what either could achieve alone.
Research consistently shows that mind-body interventions produce greater immune benefits than single-modality approaches. The HPA axis we discussed in Week 1 directly influences the physical factors we’ve covered this week. Chronic stress disrupts sleep, drives food cravings for inflammatory options, and reduces motivation for exercise. Conversely, physical practices support mental resilience.
Synergy Science: When you combine mindfulness with physical exercise, you get enhanced stress resilience. When you pair sleep optimization with stress management, you see greater improvements in immune markers than either practice alone. The whole truly is greater than the sum of parts.
5.2 Daily Integration Templates
The Morning Immune Ritual (15-20 minutes):
- Hydration (2 minutes): 16-20 oz water upon waking
- Light exposure (5 minutes): Step outside or sit by bright window
- Mindful movement (8-10 minutes): Gentle stretching or yoga with breath awareness
- Immune nutrition (timing): Include polyphenol-rich foods in breakfast
This ritual addresses hydration, circadian rhythm, stress response, and nutrition timing in one integrated practice.
Evening Integration (20-25 minutes):
- Digital sunset (ongoing): Dim lights 2 hours before sleep
- Body scan (10 minutes): Week 1 technique for physical awareness and stress release
- Sleep preparation (10 minutes): Cool room, comfortable environment
- Gratitude practice (5 minutes): Positive emotion supports immune function
Stress Response Protocol: When life hits hard, use both mental and physical tools.
- Immediate: 4-7-8 breathing (Week 1) + gentle movement
- Short-term: Increase sleep priority + reduce exercise intensity
- Recovery: Resume normal exercise gradually + maintain mindfulness practices
5.3 Troubleshooting Common Integration Challenges
Time Constraints: Life doesn’t always cooperate with ideal routines.
- Minimum effective dose: 10 minutes mindfulness + 15 minutes movement + sleep consistency
- Habit stacking: Attach new practices to established routines
- Flexibility: 80% consistency beats 100% perfection followed by complete abandonment
Motivation Fluctuations: Energy and motivation naturally vary.
- Low-energy days: Prioritize sleep and gentle movement over intensive exercise
- High-stress periods: Maintain basic practices, don’t add new challenges
- Seasonal adjustments: Adapt practices to energy and daylight availability
Social Situations: Real life includes social eating and schedule disruptions.
- Party strategy: Focus on social connection benefits, moderate inflammatory foods
- Travel adaptation: Portable versions of key practices
- Family dynamics: Model healthy practices without being preachy
5.4 Building Your Personal Immune Protocol
Assessment Tools: Before customizing, understand your unique needs.
- Energy patterns: Are you naturally a morning or evening person?
- Stress triggers: What situations challenge your immune practices most?
- Social preferences: Do you prefer group or solo activities?
- Current health status: Any conditions that require modification?
Customization Guidelines:
- Start with basics: Sleep, stress management, movement, nutrition timing
- Add one element weekly: Don’t overwhelm your system with too many changes
- Track subjectively: Energy, mood, sleep quality, illness frequency
- Adjust seasonally: What works in summer may need modification in winter
Progressive Implementation Timeline:
Week 1-2: Establish sleep consistency and basic stress management Week 3-4: Add regular movement practice and hydration habits Week 5-6: Integrate nutrition timing and fermented foods Week 7-8: Add environmental improvements and social connection Week 9-12: Fine-tune based on what’s working, prepare for seasonal changes
Section 5 Quick-Win Takeaways:
- Daily Templates: Morning immune ritual + evening integration routine
- Stress Protocol: Combined mental-physical response to challenges
- Customization: Adapt to your unique needs and circumstances
Conclusion: Your Fortress is Built, Now Maintain It
You’ve now constructed a complete immune fortress—one that operates on multiple levels to protect and strengthen your body’s natural defense systems. The mental practices from Week 1 serve as your early warning system and stress management headquarters. This week’s physical strategies provide the structural foundation: nutrition that actually impacts immune function, exercise that enhances rather than depletes your defenses, and lifestyle factors that support rather than sabotage your health.
Integration Success Metrics: You’ll know your practices are working when you notice sustained energy throughout the day, more resilient responses to stress, better sleep quality, and fewer minor illnesses. These aren’t dramatic changes—they’re the quiet confidence of a well-functioning system.
The beauty of this approach is its sustainability. These aren’t extreme measures that require perfect adherence. They’re evidence-based practices that fit into real life, accounting for busy schedules, budget constraints, and the occasional pizza party.
Your Fortress Stands Ready: But every fortress requires maintenance. The practices you’ve learned aren’t one-time fixes—they’re ongoing strategies that adapt to seasonal changes, life stress, and evolving needs. That’s what this forum targets.
Making lifestyle changes to support your greater goals.
I’ve been out of my gym at work for close to five years. We are fortunate enough to have one on facility. We’ve been working from home since the covid outbreak. I saw some familiar faces on my return. Familiar faces, yes, familiar physiques, not so much. Some have maintained a good stature while others seem to have grown, horizontally, exponentially. They didn’t make the critical lifestyle adjustments needed to maintain good physical health. I see this a lot. Good people work very hard at the gym but once they leave — the indulgences take over and eventually, no matter how hard they work at their routine, without making other lifestyle adjustments, they lose the battle for good physical health. I’m just emphasizing, nothing comes quickly but it does come eventually and then it’s just simple maintenance. And it is all about maintaining a balance of mind, body and spirit.
Coming Next Week: We’re adding the final layer to your immune fortress—the spiritual practices that science shows can literally change your cellular aging patterns. There is peer-reviewed research on spiritual connection and immune building. We’ll explore how meaning, purpose, and connection provide the final piece of your immune optimization puzzle.
Your Mission: This week, implement your integrated daily routines. Start with the basics, add one element at a time, and pay attention to how your body responds. Your immune system is about to become your most reliable ally. Also, stay mindful of your moments.
The fortress is built. Time to live in it.
Stay connected, stay well in mind, body and spirit.
Let’s have some discussion………..
- Medications and how they impact our immunities: Although we didn’t get too deep into medications, prescription drugs and over the counter medicines, are you experiencing or have you ever experienced negative immune effects from taking these types of drugs? This is a topic I’d be glad to get into, some of the research I’ve conducted indicates there are negative effects from these drugs in short use and from extended use.
- Your Personal Immune Fortress Weak Spots Looking at the five pillars covered (mindfulness, nutrition, exercise, sleep, lifestyle factors), which area is your biggest challenge and why? What’s one specific barrier that keeps you from implementing the strategies in your weakest area, and how might the community help you brainstorm solutions?
- The 80/20 Reality Check The article emphasizes that “perfect is the enemy of good” with the 80/20 approach. What does YOUR sustainable 80% look like in real life? Share your “good enough” daily routine that you can actually maintain during busy or stressful periods—let’s get practical about what consistency really means.
- Seasonal Immune Strategy Successes and Failures Winter is coming (or here, depending on when you’re reading this). What’s one immune-supporting habit that you swear by during cold season, and one that you’ve tried but failed to maintain? Bonus points for sharing your weirdest or most unconventional immune practice that actually works for you.
- The Fermented Foods Experiment The article recommends the “Rule of 3” for fermented foods—three different types, three times per week. Who’s willing to try this for the next two weeks and report back? Share your current fermented food repertoire (if any) and one new fermented food you’re willing to experiment with. Let’s create a community accountability challenge!
